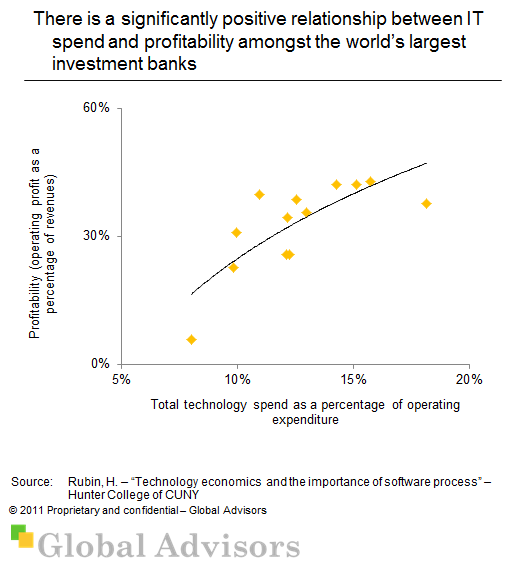
Financial services is a particularly IT intensive industry, with investment banking being the most IT intensive within it. According to data on international investment banks, those that spend more on IT as a percentage of operating expenditure typically experience higher profit margins. Can this be attributed to these banks using IT as a competitive advantage, rather than seeing it merely as a cost centre?